
The regulation of physiological bone formation and pathological soft tissue calcification
Physiological bone formation is essential for the normal functioning of the skeleton whilst pathological vascular calcification has many negative effects. This project is focused on understanding the similarities and, more importantly, the differences between these processes. This information is required to develop treatments for vascular calcification that do not cause bone loss.
Challenge
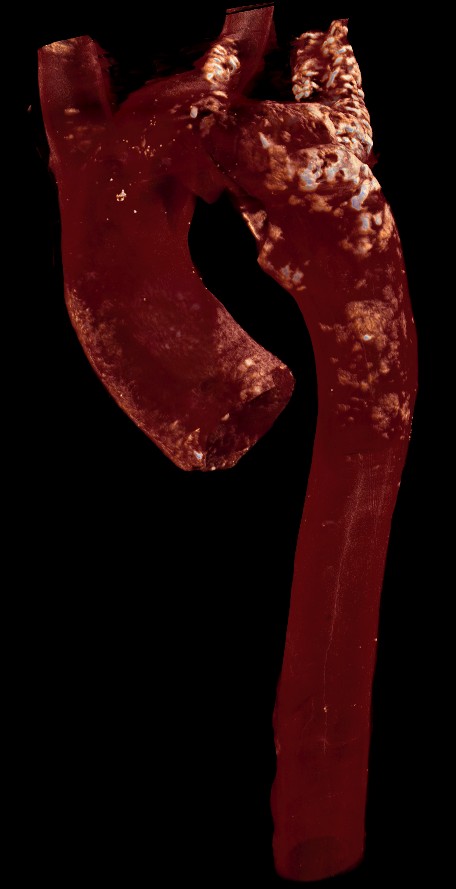
Physiological bone formation is essential for the normal functioning of the skeleton. In contrast, calcification within soft tissues has numerous negative physiological effects. Consequently, there are multiple mechanisms in place to prevent soft tissues from calcifying. When these regulatory processes fail unwanted mineral deposition can occur, a good example being vascular calcification. Vascular calcification is the formation of bone-like deposits within blood vessels and heart valves and is a significant risk factor for future adverse cardiovascular events such as heart attack and stroke.
Solution
Despite recent advances in understanding about how vascular calcification develops, there are still no effective treatments to prevent or treat this condition. Earlier research has shown that there are some outward similarities between bone formation and vascular calcification. However, targeting processes or pathways common to both processes risks off target adverse skeletal effects.
Impact
This project is focused on understanding the similarities and, more importantly, the differences between bone formation and vascular calcification. This information is required to develop treatments for vascular calcification that do not cause bone loss. In parallel, we are also working to develop novel protocols to study vascular calcification that do not use any animals or their derived products.
This research is being performed in our Camden campus, using the combined skills and expertise of vascular and skeletal biologists. This collaboration ensures that the very best, cutting edge approaches are combined with extensive knowledge of bone and vascular physiology to improve understanding in this area. Ultimately it hopes to identify novel pathways that can be targeted therapeutically to treat this serious, life threatening condition.
